Remote Patient Monitoring FAQ
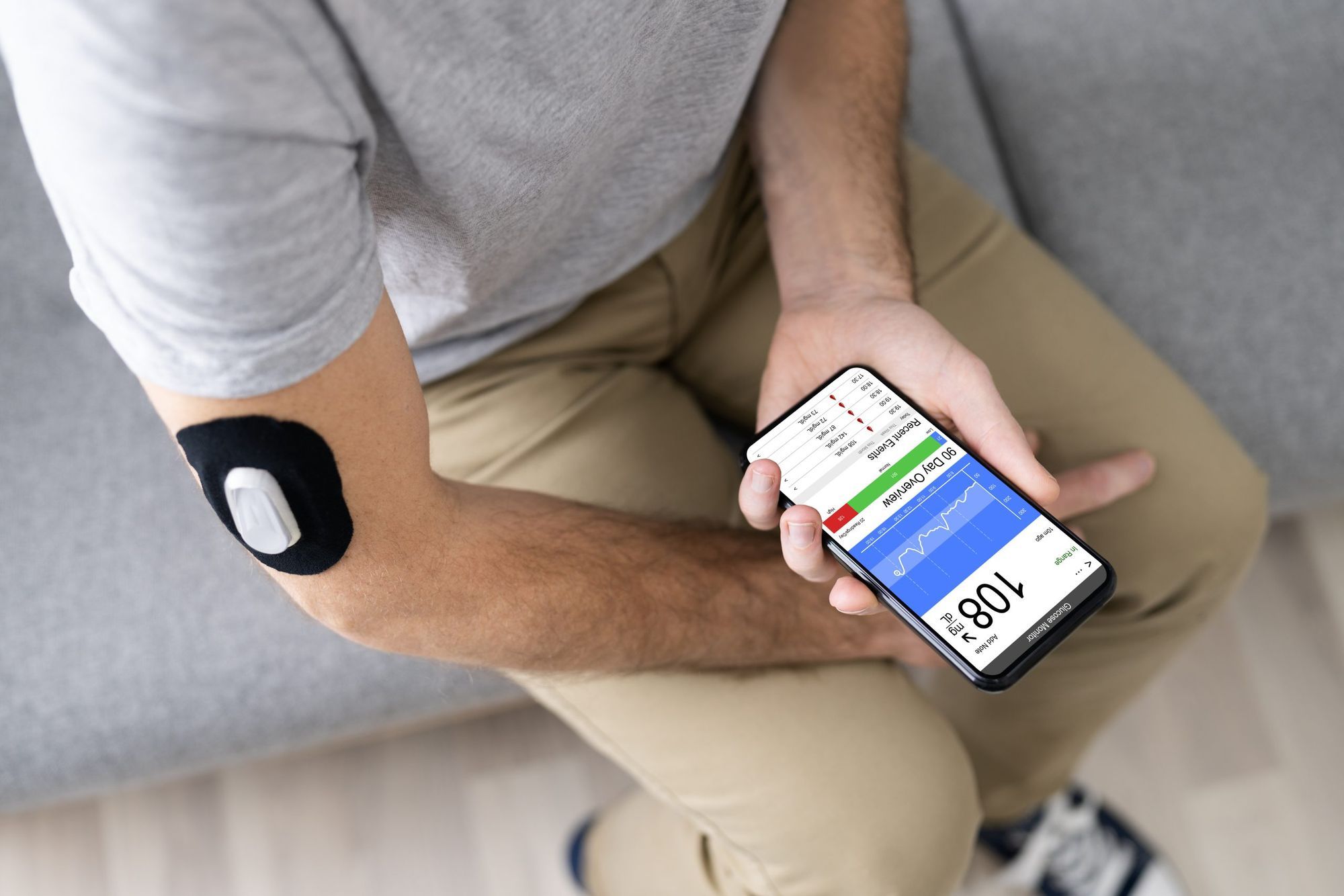
There are so many questions around Remote Patient Monitoring in research, that I decided to combine them all in this article.
If you have any further questions, please feel free to reach out.
What is Remote Patient Monitoring?
Remote patient monitoring is a method of gathering patient data outside traditional healthcare settings using information technology trends.
Examples of RPM devices:
- Blood pressure monitor
- Weight monitor
- Blood glucose monitor
- Spirometer
- Pulse oximeters
How is RPM being used in an operational setting, and why? What is the rationale for the usage of RPM in an operational setting?
There are many ways of how RPM is used in an operational setting.
One includes monitoring the patient’s condition by providers between visits. This is a great opportunity for chronic disease patients because most patients see providers once in 2-3 months, and now there is a way to track their condition between visits.
There is also detecting adverse events early to recognize signs of severe patient deterioration and hospital admission. For example, RPM can assist in fall prevention when a device immediately alerts nurses and techs when a patient attempts to exit their bed.
Moreover, facilitating care in the patient home helps patients with chronic conditions to feel more comfortable and reduce costs while having lower stress levels.
What are the common purposes for RPM research studies?
You can use RPM is perfect for monitoring patients with specific conditions to improve care. RPM is the easiest way to collect tons of data without disrupting people’s lives.
Also, you can PRO (Patient Reported Outcomes) to collect patient feedback and health state via questionnaires. It helps track the condition over time and improves patient-provider communications.
What kind of alerts are generated with RPM?
Healthcare providers can make proactive clinical decisions with real-time visibility into patient conditions.
Alerts are visual and audible messages automatically generated for a vendor’s RPM dashboard (RPM software). These alerts occur when a patient’s physiological data points exceed target ranges or thresholds set by the provider for each patient.
The provider would get an alert once there is an onset of an adverse event, such as heart failure; they would also know if the patient does not move, does not eat, or gets out of bed which could be a sign of patient deterioration.
In other cases, alerts can detect mental deterioration. RPM can help remotely monitor patients and prevent episodes of mental illness when they start to develop or track any communication issues.
What are the challenges in RPM?
- Collecting, aggregating, and reconciling data from multiple data sources and devices;
- Identifying patients and reconciling patient identities from multiple systems. For example, RPM may collect data from EHRs, proprietary devices, Fitbit, Apple HealthKit and other sources, all of which use different means to identify patients;
- Use of AI and ML as part of video monitoring to detect and alpert on adverse events has not been always reliable;
- Selecting appropriate data frequency and granularity for synchronizing data between EHRs and devices.
What are the technological processes to facilitate RPM and collect patient data?
Unlike other telemedicine delivery methods, RPM services do not require interactive audio-video or virtual visits, nor does the patient need to be in rural areas. Remote patient monitoring (RPM) devices allow healthcare providers to monitor, report, and analyze acute or chronic conditions of patients outside hospitals and clinics.
Examples:
- Communication tools: collecting patient data and feedback through PROs;
- Consumer Devices: Apple watch and/or other fitness trackers;
- Medical devices installed at home and connected to Hospital infrastructures: blood pressure monitors, weight scales, smart thermometers, and others.
- Specialized sensors: depending on a need, they can be installed in a bed, refrigerator, bathroom, and other places.
- Video monitoring equipment: if needed, there can be applications of advanced video and image recognition.
What are the new frontiers in RPM in clinical informatics?
I would say that two trends are the most important.
1. AI and ML
If a patient received a certain diagnosis, was treated with a certain medication, had certain comorbidities, and reported certain symptoms, this patient is like this other patient cohort that ended up in the ER.
Artificial intelligence can now bring insights to doctors and provide predictive skills to assist in patient care. Doctors can find it themselves, but the time and data they have to sift through to find it is very difficult in their daily work.
By using AI to provide these predictive insights as a decision support tool, physicians can make better, more data-driven decisions.
2. Real-life testing
Continuous real-time RPM is a more advanced technology that allows healthcare providers to monitor and track patient vital signs without significant delays. In the medical field, delays in treatment increase the risk of complications such as permanent disability.